|
What is Endometriosis? Endometriosis is a common women’s health condition affecting 1 in 10 women in which cells from the endometrium (lining of the uterus) appear and flourish outside the uterine cavity, usually on the ovaries. Symptoms can worsen at certain points during the menstrual cycle as cells are influenced by female hormones. Symptoms can include pelvic pain, painful periods, painful intercourse and infertility. It can also impact urinary issues and pain on urination and has been linked to interstitial cystitis. Usually endometriosis is diagnosed after a laparoscopy of the pelvic cavity although pelvic ultrasounds are also used to detect endometrial tissue outside the uterus. The shedding of endometrial tissue long term can lead to scarring and chronic inflammation which has led many experts to suggest a strong autoimmune component to the condition. In clinical practice it is something we often see coexisting with other autoimmune conditions. Risk factors for endometriosis include: family history, a diet high in trans-fats, use of intrauterine devices, and unbalanced oestrogen levels. Conventional Treatments Symptoms are often managed with hormonal medication to suppress the natural menstrual cycle, plus painkillers to manage the associated discomfort. Occasionally progesterone creams may be prescribed. The most aggressive treatment is surgery, with some women opting for a hysterectomy. The long term use of non steroidal anti-inflammatory medication for pain can contribute to the problem as it sets us up for intestinal hyper permeability (leaky gut) which adds to the picture of inflammation, so safer and effective means of reducing inflammation are needed. Although laparoscopic removal of endometrial tissue can benefit sufferers for up to 2 years, symptoms generally return and the procedure itself can cause lead to further scar tissue. In an ideal world sufferers would be referred to Nutritional Therapists or Functional Medicine practitioners to explore root cause/s and to address all angles. Natural Alternatives The naturopathic approach to endometriosis is focussed on:
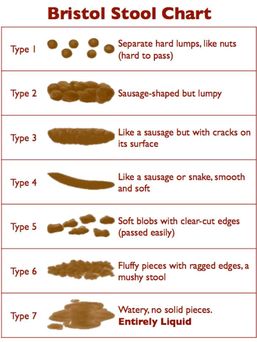
Reducing Inflammation Inflammation is a huge driver for endometriosis. The Nurses Health Study II found that women who consumed the most trans-fats (hydrogenated vegetable oils often used in processed foods) were 48% more likely to be diagnosed with endometriosis. Women with the highest consumption of omega-3 fatty acids were 22% less likely to be diagnosed with endometriosis. Reducing the amount of omega-6 fatty acids at the same time as increasing omega-3s also helps reduce inflammation. Ideally we would have an omega-6:omega-3 ratio of 3:1 however the western diet is closer to 16:1! Foods that are high in omega-6 and should be avoided include sunflower, corn, soybean and cottonseed oils. In addition to this opt for grass-fed meat as livestock fed a grain-based diet high in corn and soya produce meat high in omega-6. Foods that are high in omega-3 include: Oily fish like salmon and mackerel; flax and chia seeds; organic free-range eggs; extra virgin olive oil; and walnuts. Some people may also benefit from supplementing with an omega-3 oil in the short term while they make dietary changes. Antioxidants are very relevant to prevention and reversal of tissue damage in endometriosis, so it's important to increase our antioxidants in the diet via increasing vegetables and fruits (ideally organic). Vitamin C, A and E are beneficial and also resveratrol from red grapes, N-Acetyl cysteine, pine bark, green tea and melatonin have been studied for their powerful antioxidant benefits with some interesting results. NAC (N-acetyl cysteine ) A 2013 study of 92 women with endometriosis showed that following 3 months of supplementing with NAC for 3 days a week each week led to cancellations of laparoscopic visits due to a reduction in symptoms. A new 2023 study has also showed the benefits of NAC. Conclusions are that NAC showed a statistically significant reduction in endometriosis pain, a statistically significant reduction in endometrioma size and 75% of patients who wanted to had a spontaneous pregnancy within 6 months! I have been using NAC for a long time in clinical practice and can attest to the benefits most strongly. It also has benefits for miscarriage prevention among many others. Pycnogenol from pine bark A swiss study which gave women either Pycnogenol or GnRH (Gonadatropin releasing hormone) for 48 weeks showed a reduction in symptoms in both groups. Interestingly, after treatment stopped the benefits in the pycnogenol group lasted while the GnRH group relapsed after treatment. Melatonin A very interesting 2013 randomised, double blind placebo controlled study looked at the analgesic, antioxidant and anti-inflammatory effects of melatonin in endometriosis with some very promising results. Apart from improving sleep, melatonin was shown to reduce the risk of using analgesics by 80%. Melatonin if supplemented needs to be started slow and gradually increased up to the 10mg dose used in this study. You can also support your own natural melatonin production by avoiding the blue light effect at night from computers and TV's, wearing amber glasses and sleeping in total darkness. Certain foods such as cherry, banana, oranges, kiwi and pineapple support melatonin production as does supplementing magnesium. Enhancing Detoxification Yes, we are talking about poo here! Actually detoxification involves the gut and the liver but it’s vitally important to make sure that we move our bowels at least once every day if we want to facilitate optimal detoxification. We also want to make sure that we are having a normal bowel movement. On the Bristol stool chart below we should be aiming for a 3-4. If you are having anything other than that pop in and have a chat because there are lots of things you can do to support healthy bowel function. Constipation is a common problem in hormonal imbalance across the board and we need to get to the root cause to eliminate this risk factor properly. Increasing the amount of vegetable-based fibre in the diet is vital if we want to support our gut bacteria as this is what the good bacteria feed on. Increasing our intake of vegetable fibre has been shown to help clear excess oestrogen from the bloodstream. Cruciferous vegetables are particularly good at this so increase your intake of: broccoli, brussels sprouts, cabbage, kale and cauliflower. Supplementing with the right B vitamins can support detoxification of hormones promoting balance. Endometriosis often involves higher oestrogen over progesterone (which tends to be low), another commonly used herbal supplement which is used to rebalance the hormones is Agnus castus. There are further supplements which support this but these are advised on a case by case basis and depend on identifying individual challenges and possibly further testing. For some sufferers there may be an underlying SIBO (small intestine bacterial overgrowth) which needs to be dealt with. Balancing hormones This involves diet as well as removal or avoidance of a class of chemicals known as endocrine disrupters. That's because these chemicals found in our cleaning fluids, toiletries and cosmetics and plastic bottles actually exert a xeno-oestrogen or oestrogen mimicking effect. The trouble is our bodies don't know the difference between a real oestrogen and a pretend one so exposure to these chemicals needs to be avoided if we want to balance hormones. The increased exposure to these endocrine disrupters in modern living explains in part the increased challenges with many hormonally driven conditions. So time to take a look at your bottles hiding under the sink and examine your toiletries. There are many alternatives available which avoid all the nasties such as parabens and phthalates etc. Using essential oils are a safer way to clean your home and good old fashioned vinegar and bicarb will save you money and unnecessary toxin exposure. Managing stress Hormones don't work in isolation. The endocrine system works as a team and managing our stress hormones is key to supporting any hormone challenges. It's also why a comprehensive assessment of stress hormones is included in my preferred hormone screening. When stress is chronic and cortisol is elevated, progesterone can drop leading to unpleasant symptoms such as moodiness, increased weight around the middle, sleep problems and breast tenderness. Supplementing with magnesium and adaptogen herbs can support this as can meditation, yoga and mindfulness. Reducing Symptoms Studies have shown a significant reduction in symptoms in women who move away from eating higher-glycaemic carbohydrates (bread, pasta, rice, cakes, etc.), reduce caffeine and increase their intake of Omega-3 fatty acids. Caffeine can have be a problem for many women with endometriosis with one study showing consuming 150-225mg of caffeine per day (about 1-1.5 cups of coffee) increased the risk of endometriosis by 20% and those who drank more than 225mg of caffeine had a 60% increase. Supporting blood sugar balancing is fundamental for hormone balancing as these two are related. Turmeric has been shown to reduce inflammation, support blood sugar (important when you’re trying to reduce food cravings), reduce pain and support liver detoxification making it a key supplement in the support of endometriosis. Magnesium, Ginger root and Devil's claw are also favourites as anti-inflammatories in place of NSAID's. Magnesium can be taken throughout the month with an increased dose the week prior to a period. Magnesium is commonly deficient in endometriosis and you may be experiencing symptoms of deficiency such as twitchy eyes, restless legs, anxiety, palpitations, headaches, sleep problems. These are things I see commonly in clinical practice. It's important to find the right kind of magnesium and also the right dose for you so do get in touch to find out more. A simple way of using it in addition to oral supplementation is to use a spray on the abdomen daily and increase the week before a period. In addition to its anti-inflammatory benefits, magnesium is also essential for energy, mood, sleep and blood sugar regulation. We also recommended epsom salt baths due to very good transdermal absorption. Food intolerance also play a part here in that if we continue to eat foods which we are intolerant to we add to the picture of inflammation. One of the biggest drivers in endometriosis is gluten and studies have shown a significant reduction in symptoms following a gluten free diet. However, when IgG food intolerance testing is done, we can see a further reduction in symptoms. Other food triggers can be dairy, soya, yeast, eggs, corn, peanuts, cane sugar and also foods in the nightshade family eg tomatoes, potatoes etc. Endometriosis has a strong link with IBS so following the anti-inflammatory protocol above and an elimination has been found to be supportive of both conditions. Genetics: nutrigenomics is the study of how nutrition influences every aspect of our gene expression. When we do genomic testing we learn how our individual genetics play a role in every aspect of our physiology from detoxification to how we metabolise hormones and nutrients (among many others) and this is becoming such a pivotal starting point for many as it gives use those immediate signposts at an individual level as to why a person may need more specific support with certain supplements or why they may not tolerate others. It can also guide us to the right type and combination of supplements when we know the individual needs based on genetics. We also learn how our nutrition influences our gene expression either positively or negatively so we can make the most optimal choice for us. If you're one of those people who feels they have tried everything and is still not getting the answers and symptoms resolution, looking at genetics could definitely be the way forward. You could always book a discovery call if you would like to understand more. Massage therapy can also help reduce symptoms. An Iranian study showed that massage of the back, sacrum and abdomen lead to a significant reduction in painful dysmenorrhea caused by endometriosis. Abdominal massage can also stimulate peristalsis in the large intestine therefore support detoxification. In addition to this abdominal massage can also help to breakdown scar tissue and adhesions. In all cases risk factors and drivers are always individual and an appointment with a Nutritional Therapist can help you uncover the triggers and drivers of your own condition and support you with an individualised protocol. We also have access to a range of tests including comprehensive hormone screening such as the DUTCH Test which covers reproductive hormones, stress hormones, melatonin levels, neurotransmitters and B vitamin metabolites. We can also assist you with long term plans such as fertility and other co-existing health challenges. Always ask us first before choosing supplements as there may be drug nutrient interactions to consider or speak to your healthcare provider. Some off the shelf supplements may also contain food allergens and other additives. To book an appointment or for enquiries contact us here References: https://academic.oup.com/aje/article/137/12/1353/155016 http://cancerres.aacrjournals.org/content/41/9_Part_2/3771.short http://www.fertstert.org/article/S0015-0282(01)01991-4/abstract https://academic.oup.com/humrep/article/25/6/1528/2915756 http://europepmc.org/abstract/med/23334113 https://www.sciencedirect.com/science/article/pii/S0753332217346838 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3093183/ https://www.ncbi.nlm.nih.gov/pubmed/17879831 https://www.ncbi.nlm.nih.gov/pubmed/23737821 https://www.ncbi.nlm.nih.gov/pubmed/23602498 https://pubmed.ncbi.nlm.nih.gov/18983759/ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10048621/
2 Comments
6/11/2019 08:43:09 pm
I didn't know that endometriosis can be caused by a diet high in trans-fat. My friend started feeling unusual pain during her periods and was diagnosed with endometriosis. I believe that my friend can be cured, but she should start eating healthy since diet is one of the main contributors to her disease. I'll make sure to cook for her so I can also monitor her diet.
Reply
Leave a Reply. |
Amazon Associates DisclosureNourishing Insights is a participant in the Amazon EU Associates Programme, an affiliate advertising programme designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.co.uk. Archives
December 2023
|
WHAT OUR CLIENTS ARE SAYING“I did Nutritional Therapy with Beverley and it was life changing. I highly recommend it!” Allison Blakely (Glasgow)
|
Contact Us |